When panic hits-heart racing, breath gone, mind spinning-benzodiazepines can feel like a lifeline. For many, a single dose of alprazolam or lorazepam stops a panic attack cold. But what happens when that lifeline becomes a chain? These drugs are powerful, fast-acting, and dangerously easy to misuse. They’re not just pills; they’re chemical tools that alter how your brain works, and that comes with serious trade-offs.
How Benzodiazepines Work
Benzodiazepines don’t just calm you down-they quiet your brain’s overdrive. They bind to GABA receptors, the brain’s main braking system. GABA is the neurotransmitter that tells neurons to slow down. When benzodiazepines latch onto these receptors, they make GABA work harder. The result? Less electrical noise in the brain. That’s why they reduce anxiety, stop seizures, relax muscles, and induce sleep. The effect is fast: within 30 to 60 minutes, you feel it. No waiting weeks like with SSRIs. That speed is why doctors still prescribe them for acute crises-like panic attacks, alcohol withdrawal, or pre-surgery anxiety.
Common Uses and Which Drugs Do What
Not all benzodiazepines are the same. They’re grouped by how long they last in your body, and that determines their use.
- Short-acting (like triazolam and midazolam): Used for sleep or sedation before procedures. They leave your system fast, so you don’t feel groggy the next day.
- Intermediate-acting (like lorazepam and alprazolam): The go-to for panic and anxiety. Alprazolam (Xanax) is one of the most prescribed. It works fast and wears off in a few hours, making it good for sudden spikes in anxiety.
- Long-acting (like diazepam and flurazepam): Used for chronic conditions like alcohol withdrawal or muscle spasms. Diazepam (Valium) sticks around for days, which helps smooth out withdrawal symptoms but increases risk of next-day drowsiness.
The FDA has approved specific drugs for specific uses. Midazolam is the standard for emergency seizure control. Chlordiazepoxide (Librium) is used for alcohol detox. Flurazepam is only for insomnia. Each drug is chosen based on timing, strength, and how long the effect needs to last.
The Real Benefits: When They Save Lives
These drugs aren’t just for anxiety. In emergencies, they’re irreplaceable. In the ER, when someone is having a seizure that won’t stop, midazolam or diazepam can shut it down in minutes. In the ICU, they keep ventilated patients calm. For people going through alcohol withdrawal, benzodiazepines prevent deadly seizures and delirium. Studies show they’re 60-80% effective for acute anxiety-far faster than antidepressants, which take weeks to kick in. For someone in a full-blown panic, that speed is everything. One Reddit user described alprazolam as “the only thing that stopped my heart from trying to crawl out of my chest.” That’s not hyperbole. For short-term, targeted use, benzodiazepines work.
The Hidden Risks: Dependence and Withdrawal
Here’s the catch: your brain adapts. After just 2-4 weeks of daily use, your GABA receptors start to downsize. You need more of the drug to get the same effect. That’s tolerance. Then comes dependence. The WHO says 30-50% of people taking therapeutic doses for more than four weeks become physically dependent. That means your body expects the drug to function normally. Stop suddenly, and your brain goes haywire.
Withdrawal isn’t just feeling jittery. It’s the opposite of the drug’s effect-amplified. People report severe anxiety, insomnia, tremors, muscle pain, hallucinations, and even seizures. A 2022 survey found 23% of users had memory gaps during normal daily activities. That’s anterograde amnesia-forgetting events as they happen. It’s not rare. One user on r/PharmaCon described 11 months of withdrawal after 12 years of use: “I lost my job, my relationships, and nearly my life.”
Why Long-Term Use Fails
Benzodiazepines don’t cure anxiety-they mask it. And when you rely on them long-term, you miss the chance to learn how to cope. Cognitive behavioral therapy (CBT) for anxiety or insomnia (CBT-I) has lasting results without any drugs. A 2023 JAMA study found that combining low-dose benzodiazepines with CBT cut dependence risk by 58%. But if you skip the therapy? You’re just delaying the crash. The American Psychiatric Association recommends no more than 2-4 weeks of continuous use. Yet, in the U.S., 12.6% of adults got a benzodiazepine prescription in 2021. Many took them for months or years. That’s not treatment. That’s risk.
Who’s Most at Risk?
Women are prescribed benzodiazepines more often-8.3 prescriptions per 100 women versus 4.3 per 100 men. Why? Partly because anxiety disorders are diagnosed more in women. But also because doctors sometimes default to prescribing rather than referring to therapy. Older adults are another high-risk group. The American Geriatrics Society warns against using benzodiazepines after age 65. They increase fall risk by 50% and raise dementia risk by 32%. One study found that seniors on long-term benzodiazepines had twice the chance of ending up in the ER after a fall. And yet, they’re still prescribed.
Alternatives That Work Better Long-Term
Antidepressants like SSRIs and SNRIs take longer to work-4 to 6 weeks-but they’re safer for ongoing use. They don’t cause dependence, and they address the root of anxiety, not just the symptoms. For sleep, CBT-I is more effective than any sleeping pill, including Z-drugs like zolpidem. For panic, exposure therapy rewires fear responses without drugs. Even mindfulness and regular exercise reduce anxiety over time. The problem isn’t that benzodiazepines don’t work. It’s that they work too well in the short term, making it easy to forget they’re not a long-term solution.

How to Use Them Safely
If you’re prescribed a benzodiazepine, ask these questions:
- What’s the goal? (e.g., “I need this for one panic attack before my flight”)
- How long am I allowed to take it? (Never more than 2-4 weeks without reevaluation)
- Is there a taper plan if I need to stop?
Never stop cold turkey. Withdrawal can be deadly. The Ashton Manual-the gold standard for tapering-recommends reducing your dose by 5-10% every 1-2 weeks. For someone on long-term use, that can take 3 to 6 months. Some need a year. Your doctor should be trained in this. In the U.S., psychiatrists must complete 40 hours of continuing education on controlled substances every two years. If your prescriber hasn’t done this, ask why.
The Bigger Picture: Why Prescriptions Are Changing
Prescription rates are falling in places that act. Kaiser Permanente cut long-term benzodiazepine use by 37% by adding alerts in their electronic records when prescriptions go over 90 days. France still has the highest use-78 doses per 1,000 people daily. The U.S. is at 12. The UK’s NICE guidelines now say: don’t start benzodiazepines for anxiety. The FDA added a boxed warning in 2020 about abuse, addiction, and withdrawal. The DEA still classifies them as Schedule IV-meaning they’re controlled but available. But the trend is clear: these drugs are being pushed to the edge of medicine, reserved only for emergencies and short-term crises.
What to Do If You’re Already Taking Them
If you’ve been on benzodiazepines for more than a month:
- Don’t panic. Dependence doesn’t mean failure.
- Don’t stop on your own.
- Find a doctor who knows how to taper safely. Look for someone trained in addiction medicine.
- Ask about CBT or other therapies to support the process.
Many people successfully taper and regain control. But it takes time, support, and patience. The goal isn’t just to stop the drug-it’s to rebuild your brain’s natural ability to handle stress.
Can benzodiazepines be used safely for long-term anxiety?
No. Benzodiazepines are not safe for long-term anxiety management. Tolerance builds within 2-4 weeks, meaning higher doses are needed for the same effect. Physical dependence develops in 30-50% of users after just four weeks of regular use. Long-term use increases risks of cognitive decline, falls (especially in older adults), and severe withdrawal symptoms. Guidelines from the American Psychiatric Association and NICE recommend avoiding benzodiazepines for chronic anxiety. Alternatives like SSRIs and CBT are safer and more effective over time.
How fast do benzodiazepines work?
Benzodiazepines work quickly-usually within 30 to 60 minutes after taking them orally. This makes them ideal for sudden anxiety, panic attacks, or pre-procedure sedation. For example, alprazolam (Xanax) reaches peak levels in the blood in about 1-2 hours. Fast-acting forms like intramuscular or IV midazolam can stop a seizure in under 5 minutes. Their speed is their biggest advantage, but also why they’re so risky for regular use.
What are the most common side effects?
Common side effects include drowsiness, dizziness, fatigue, impaired coordination, memory problems, and confusion. Some people experience increased anxiety, agitation, or muscle weakness. Long-term use can lead to cognitive decline, falls, and anterograde amnesia-forgetting events that happen while under the drug. A 2022 survey found 23% of users reported memory gaps during daily activities. These effects worsen with age and when combined with alcohol or opioids.
Can you overdose on benzodiazepines?
Isolated benzodiazepine overdoses are rarely fatal on their own-they don’t suppress breathing as severely as opioids. But they become deadly when mixed with alcohol, opioids, or other sedatives. In 2021, benzodiazepines were involved in over 11,000 U.S. overdose deaths, mostly when combined with opioids. Even at prescribed doses, combining them with other depressants increases risk. That’s why doctors now screen for substance use before prescribing.
What’s the difference between dependence and addiction?
Dependence means your body has adapted to the drug and will experience withdrawal if you stop. It’s a physical state, even with proper use. Addiction involves compulsive use despite harm-cravings, loss of control, using for reasons beyond medical need. Many people become dependent without being addicted. But dependence can lead to addiction if someone starts taking more than prescribed to avoid withdrawal or chase the initial high.
Are there non-drug alternatives that work as well?
For long-term anxiety and insomnia, yes. Cognitive behavioral therapy (CBT) is as effective as benzodiazepines for panic and anxiety, and more effective over time. CBT-I (for insomnia) has lasting results without side effects. Exercise, mindfulness, and sleep hygiene also reduce anxiety naturally. While benzodiazepines offer instant relief, these methods build lasting resilience. A 2023 study showed combining low-dose benzodiazepines with CBT cut dependence risk by 58%. The best approach is short-term use with therapy-not long-term reliance on pills.
These drugs have a place in medicine-but only in the right hands, for the right reasons, and for the right amount of time. They’re not a cure. They’re a bridge. And bridges are meant to be crossed, not lived on.

 Allergic Reactions to Generics: When to Seek Medical Care
Allergic Reactions to Generics: When to Seek Medical Care
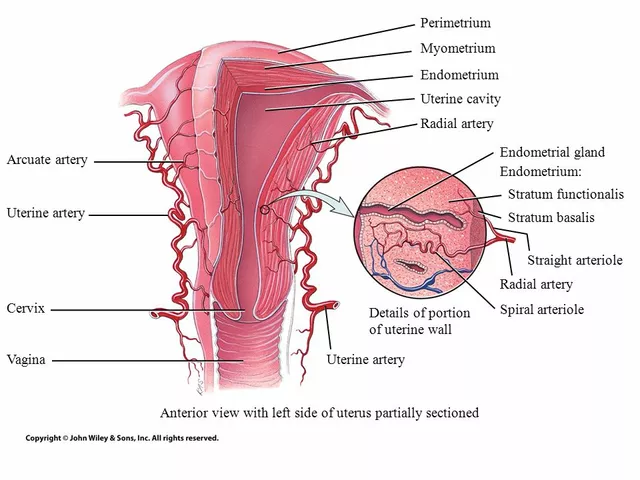 The Connection Between Overgrowth in the Uterine Lining and Migraines
The Connection Between Overgrowth in the Uterine Lining and Migraines
 OTC Diarrhea Treatments: When to Use and When to See a Doctor | Safe Self-Management Guide
OTC Diarrhea Treatments: When to Use and When to See a Doctor | Safe Self-Management Guide
 Vertigo and Dizziness: Understanding Inner Ear Disorders and How Vestibular Therapy Helps
Vertigo and Dizziness: Understanding Inner Ear Disorders and How Vestibular Therapy Helps
 Why Your Pills Look Different: Safety, Legality, and What Patients Need to Know
Why Your Pills Look Different: Safety, Legality, and What Patients Need to Know
Sarah B
February 7, 2026 AT 19:27Benzos are just another drug the government lets Big Pharma push to keep us docile
Patrick Jarillon
February 9, 2026 AT 00:02Oh wow so now we're supposed to believe the FDA and APA? LMAO. They're in bed with pharma. I've been off benzos for 8 years and my brain finally stopped screaming. They don't treat anxiety-they rewire your soul to need chemicals. And don't get me started on how they're used in prisons and psych wards to shut people up. This isn't medicine. It's chemical control. You think you're calming down? Nah. You're being muted. And the docs? They're just the gatekeepers for the machine.
My cousin took Xanax for 'stress' for 3 years. Now she can't sleep without 4mg. She's 28. They told her it was 'safe.' Safe like a loaded gun in a toddler's room.
CBT? Yeah right. Who's gonna pay for that when a script costs $15 and takes 5 minutes? The system doesn't want you healed. It wants you compliant. And benzos? Perfect for that.
They're not bridges. They're quicksand. You think you're crossing? You're sinking. And they'll tell you it's 'normal' until you're too far gone to scream.
Niel Amstrong Stein
February 9, 2026 AT 07:55Man I remember when I first tried lorazepam after a panic attack at work. Felt like someone turned off a hurricane inside my chest. Like, literally stopped breathing for a sec because it was too calm.
But then I got lazy. Took it for a flight. Then for a bad day. Then for... just because. Didn't even realize I was dependent until I tried to quit and my hands shook like I was in an earthquake.
Now I do yoga, cold showers, and journaling. Took 6 months. Felt like climbing a mountain barefoot. But I didn't lose myself. And I actually sleep better now. No pills. Just me. Weird, right?
Still take one once in a blue moon. Like a backup generator. Not the main power.
Also 🙏🙏🙏
Heather Burrows
February 10, 2026 AT 22:14So let me get this straight. We're supposed to trust a bunch of doctors who prescribe these like candy, then suddenly act shocked when people get hooked? Please. I work in ER. We see the same people every month. 'I lost my script.' 'I ran out.' 'I need more.' They're not addicts. They're patients. And we're failing them.
CBT is great. But what if you can't afford it? What if you have 3 jobs and no insurance? What if your therapist won't take Medicaid? You think they're choosing this? No. They're choosing survival.
Stop blaming the people. Start fixing the system. Until then, don't act like you're saving lives by taking away the only thing that keeps them from screaming into the void.
Lakisha Sarbah
February 12, 2026 AT 02:46im 32 and been on xanax for 7 years. not addicted. just need it. like insulin. dont judge. just sayin.
Paula Sa
February 13, 2026 AT 01:59I want to say thank you to whoever wrote this. I was on diazepam for 4 years after my mom died. I thought I was coping. Turns out I was just numbing. When I finally tapered slowly with my psychiatrist's help, I cried for three weeks straight. But then... I started feeling things again. Real things. Sadness. Joy. Anger. Even boredom.
It wasn't pretty. But it was mine. And now I go to therapy twice a week. I run. I cook. I breathe. I'm not 'cured.' But I'm alive. And that's more than I can say for the version of me on benzos.
If you're reading this and you're stuck-please don't give up. Healing isn't fast. But it's possible. You're not broken. You're just tired.
Marcus Jackson
February 14, 2026 AT 06:31lol you think CBT works? i tried it. therapist asked me why i was anxious. i said 'because my job is hell and i make 15k a year.' she said 'let's reframe that.' i walked out. no thanks. i'll take the pill.
Mary Carroll Allen
February 14, 2026 AT 13:24wait so if benzos are so dangerous why are they still on the WHO essential meds list?? and why do they use them in ERs for seizures?? if they're that bad, why are they the FIRST line of defense??
they're not perfect. but they're not evil. they're tools. like a scalpel. you can cut yourself with it or you can save a life. context matters.
also i got off after 5 years. took 8 months. i did cbt. i meditated. i ran. i cried. i screamed into a pillow. i got a dog. i got a job. i'm not 'better.' i'm just not a zombie anymore.
to everyone still on them: you're not weak. you're surviving. and you deserve better than shame.
Joey Gianvincenzi
February 16, 2026 AT 09:56It is with profound gravitas that I must address the systemic moral failure inherent in the contemporary pharmacological paradigm, wherein the commodification of neurochemical tranquility has supplanted the cultivation of existential resilience. The pharmaceutical-industrial complex, in its insidious omnipresence, has engineered a societal dependency predicated upon the illusion of expedient solace, thereby obviating the necessity for authentic psychological integration. One cannot, in good conscience, endorse the administration of a substance whose primary therapeutic mechanism is the suppression of human affective response, rather than the restoration of homeostatic equilibrium through cognitive and behavioral reconditioning. The very notion of long-term benzodiazepine utilization constitutes a metaphysical abdication-a surrender of agency to molecular manipulation. One must ask: if the mind is silenced, is the soul still speaking?
Tola Adedipe
February 17, 2026 AT 16:37Joey just said that and I’m crying. Not because I agree. But because he’s right. And that’s the scariest part.
My sister died last year. Overdose. Mix of benzos and fentanyl. She was 34. Took them for anxiety since she was 21. Her doctor never mentioned tapering. Never asked if she had support. Just renewed the script. Every month.
She didn’t need a philosopher. She needed someone to ask: ‘What’s going on?’ Not ‘Here’s a pill.’
So yeah. I agree with Joey. But I also agree with Lakisha. And Heather. And Niel. And Patrick. We’re all right. And we’re all broken. And that’s why this isn’t about drugs. It’s about care.